The use of pulse oximetry at home has expanded over the past 20 years as the population ages and the incidence of respiratory and cardiac diseases increases. A pulse oximeter is a noninvasive prescription medical device used for measuring a patient’s oxygen level (SpO2) in the blood and pulse rate. These are important vital signs to provide feedback on a patient’s health status; accurate readings are crucial. Selfmonitoring using pulse oximetry enables patients with conditions such as chronic obstructive pulmonary disease (COPD), asthma, congestive heart failure (CHF) and those on long-term oxygen therapy to more actively manage their day-to-day conditions.
Home pulse oximetry monitoring also helps caregivers or clinicians determine if the therapeutic goals are being met. Pulse oximetry monitoring and spot-checking
from home can save time, anxiety and doctors’ visits, and, in general, helps patients with respiratory disease live an active and independent lifestyle1. Home pulse oximetry will play an even more important role in remote clinical decision making and potentially improve patient outcomes as the population continues to age and live independently. The following are five things every HME provider should know about oximetry.
How Does Pulse Oximetry Work?
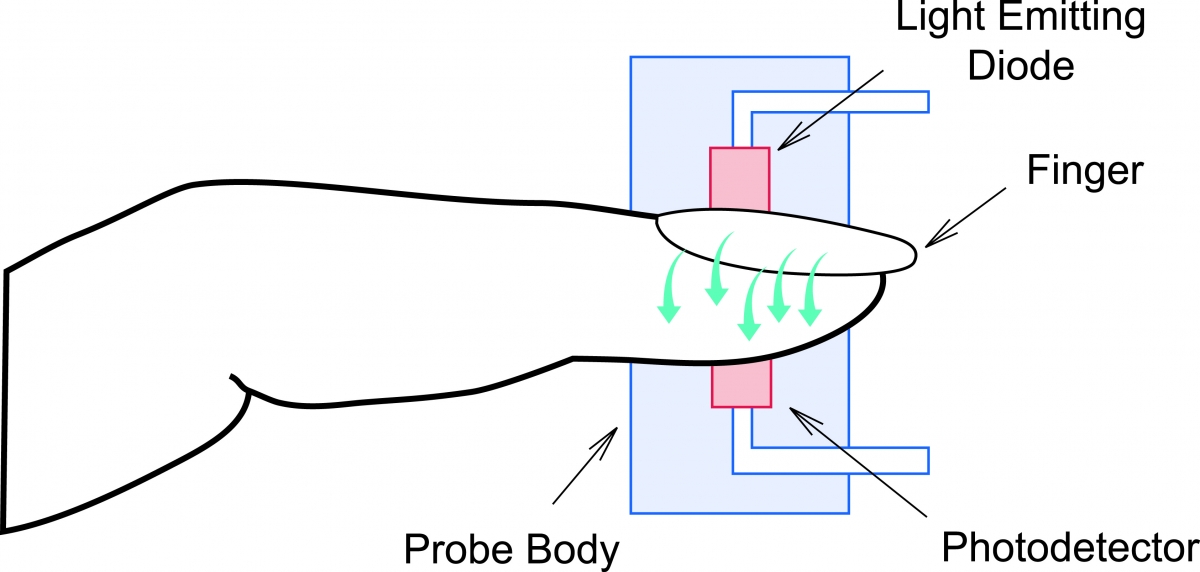
A pulse oximeter, usually attached to the finger, shines two separate light beams into the blood circulating in the small vessels, i.e., capillaries. These light beams reflect the amount of oxygen in the blood, expressed as a percentage, along with the pulse rate. Oxygen saturation (SpO2) measures how much oxygen the blood is carrying.
What Are the Benefits of Using a Pulse Oximeter?
A pulse oximeter can provide objective information about health care status to the patient or health care provider. Having impartial data to reference in addition to the patient’s subjective feedback (e.g. symptoms) may help the caregiver determine health condition and the possible need for medical consultation or intervention.
Additionally, finger oximeters can be used during a clinician-prescribed exercise routine to provide instant and accurate readings. If individuals are able to stay well-oxygenated while moving, pulse rates are less likely to reach excessively high levels, and the patient should be able to complete activities more comfortably.
What Type of Pulse Oximetry Device Is Needed?
The type of patient being monitored, along with the complexity of the medical situation, can help drive the decision to use a simple spot-check device versus a continuous, alarmed device. With a prescription, a saturation level is given for the alarm setting. As operating environments vary, be sure to use caution to ensure that all audible alarms and indicators can be heard. A patient in a more severe state, such as one who has dependence on a ventilator or life-support system, is more likely to require continuous pulse oximeter monitoring through the use of a tabletop or hand-held device. Spot check finger pulse oximeters are usually sufficient for patients who are ambulatory and want to monitor levels during activity or a few times a day.

Patients with chronic respiratory diseases like COPD, asthma or CHF, or who are reliant on supplemental oxygen usually find a spot check device meets their needs to be active, independent and confident in their day-to-day health status. If spot checks are sufficient, proven finger pulse oximeters are useful in providing assurance and peace of mind to the patient and family.
What to Look for in a Spot-Check Oximeter?
Finger pulse oximeters are ideal for spot checks and are portable, battery operated and user friendly. However, other factors should be considered, such as confidence in the reliability of the oximeter long-term as well as the belief in the accuracy of the device in challenging patients. A lot of oximeters are on the market, and any oximeter may work well on a certain patient, but it is the challenging patient population like those with chronic conditions who require the most accurate data to aid in better and faster decision making. Patients with chronic diseases usually suffer from low blood flow (e.g. perfusion), which can impact accuracy. It is important to ask the manufacturer for proven accuracy claims backed by evidence such as published clinical papers. Good pulse oximeters will have specific labeling for challenging conditions.
Here are some factors to consider:
Ideal Features and Functions for Spot-Check Oximeters2
Feature
• Small and portable
• Lightweight
• Easy to use: automatic on/off, simple battery changes, easy-to-read results
• Flexible fit—all finger sizes from adult to pediatric
Function
• Reliable—meets ±2 accuracy with proven clinical data
• Works with a variety of blood pressures and perfusion levels
• Accurate to 70% saturation
• Accurate with some motion
• Durable—able to withstand drops and some moisture
What Are the Limitations of Pulse Oximetry?
Although the noninvasive nature of pulse oximetry has added value in the homecare setting, it does have some limitations. As with any medical device, the use of pulse oximetry and the limitations for the patient should always be discussed with the patient’s doctor.
Pulse oximeters are available at reasonable price points and are an easy-to-use, timesaving device that can enhance patient care at home and quality of life.
*Sources: 1. Clinical Use of Pulse Oximetry Pocket Reference
2010. WONCA/ICC. 2. Koff PB. Pulse Oximetry at Home. White
Paper. May 2010
Senior Care Products, Winter 2011
