
Lexi lost both kidneys to cancer at 17 months. Allison was born with a condition that progressively robbed her of the ability to breathe and grow. And at 6-days-old, Lucas had surgery to remove most of his large intestine.
Thirty years ago, these children would likely have been hospitalized for long periods of their lives—if they survived at all.
Today, children with medical complexities not only survive, they live full lives at home rather than in a hospital. While home care is most often associated with the elderly, thanks to advanced technology and techniques, more and more medically complex children have the option to live at home and be part of the community.
That was not true 25 years ago. There were no in-home health services tailored to meet the needs of children with complex medical conditions when Pediatric Home Service (PHS) opened its doors in 1990. The demand for pediatric home care has since grown substantially, along with the array of services, providers and technology. Today, the pediatric population thought to have special health care needs ranges from 0.7 percent (those with highest level of medical complexity and need) to 18 percent (anyone who falls in the "children and youth with special health care needs" category).
At the same time, aging baby boomers are contributing to a growing need for home care services. By 2017, the over-65 population will be greater than the under-five population for the first time in history, putting more strain on an industry already competing for too few resources, particularly skilled professionals.
The evolving segment of pediatric home care is facing multiple challenges, including a lack of fair payment for services, restrictive coverage and benefit exclusions, shortages of home health nurses with pediatric expertise, a lack of meaningful data on the complex pediatric population, and even a lack of a clear understanding of how pediatric home care will integrate into the overall health care system in the future. These challenges must be addressed—not only to ensure access to high quality home care for medically complex children, but as part of an overall solution to remedy our nation's health care problems. Home-based care for all ages is increasingly seen as a strategy to help achieve the Triple Aim of the U.S. health system outlined in the Affordable Care Act, which is to improve the health of the population, lower total cost of care, and improve the patient experience.
Here is a look at what our industry can do to help make sure that happens.
Define and Differentiate Pediatric Home Care Services
The name seems self-explanatory, but pediatric home care includes a wide range of services not always understood or recognized. Services can be as simple as a home health aide regularly assisting with patient daily living activities or as complex as a highly trained nurse administering and monitoring infusion therapy or skilled assessments and interventions. Staff in different disciplines with advanced skill levels move in and out of a home in shifts. Comprehensive care plans and designation of essential skill level requirements are critical in caring for children with medical complexities. Family caregivers are also trained by these clinicians to deliver appropriate care.
 Pediatric home health providers deliver needed stimulation in all areas of a child's development.
Pediatric home health providers deliver needed stimulation in all areas of a child's development.The challenge for pediatric home care providers is to put the right people in the right places with the right resources for the best possible outcomes for patients and their families. As the market expands for a variety of home care services—including the provision of sophisticated medical devices commonly referred to as durable medical equipment (DME)—roles, qualifications and services must be clearly defined to make sure patient needs are met.
Adequately Reimburse Services
Payment must be sufficient to allow specialized home care companies to deliver evidence-based care consistent with pediatric medical standards. Medicare rates—not Medicaid—are used as the basis for pricing applied to DME, supplies and home health services for most payers, yet treating a pediatric patient as if they were a geriatric patient would yield catastrophic results. Our challenge as providers is to highlight the differences for all stakeholders, so that we are assured fair compensation for care provided.
Other reasons that current reimbursement rates and regulations haven't kept pace include:
- A lack of awareness among payers and policy makers of the complexity and variety of pediatric home care products and services, and the costs incurred in their delivery. Some payers use the "lower the total cost of care" to justify their significant rate compression.
- Insurance coverage that does not account for the comprehensive nature of home health services.
- State coverage and Medicaid payment that varies greatly from state to state.
- No standard definition of what constitutes "medically necessary care."
The payment system for pediatric home health care is a model in need of change, one that recognizes the unique nature of pediatric home care.
Recruit and Retain Professionals
Home health care resources—particularly the number of skilled or experienced professionals—are in short supply. It's a situation that will worsen as the aging population creates even greater demand for home health care services.
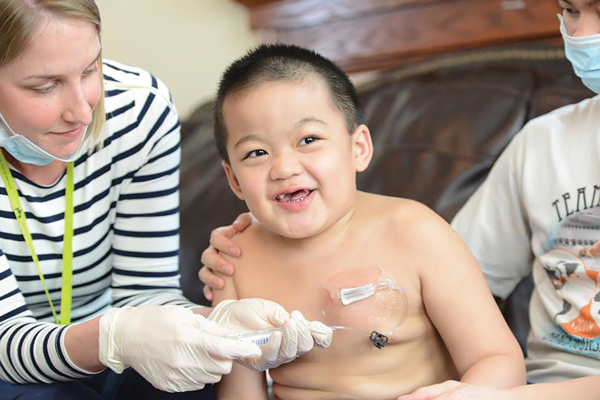 A pediatric home health nurse administers medication through a port
A pediatric home health nurse administers medication through a portIn Minnesota, we are lucky to graduate more nurses than there are positions open. But these nurses have many opportunities and they often want hospital experience. Some of this can be attributed to wages, but the environment is also different. Because hospital nurses see a wide variety of patients, it is perceived that they get to use assessment skills more and learn about a variety of different diseases, making it an attractive option. How do we attract nurses to careers in home health care?
It is important to make sure people understand that home care is a specialty. It requires a single nurse or professional to apply a broad set of skills to perform all the services and care. Home health nursing is a meaningful, challenging and rewarding career with plenty of opportunities to grow. At PHS, we partner with area colleges and universities to provide nursing students with learning opportunities ranging from an introduction to the field to a more in-depth experience that includes job shadowing and hands-on care. In 2015, we sponsored a pediatric nursing conference with leading Minnesota physicians and focused on the evolving home health care market.
Additionally, the industry must advocate for pay that crosses all locations of care and compensates home care nurses for what they do, not where they do it. Home care nurses provide intensive and appropriate care for patients with medical complexities on a daily basis. They are highly trained and skilled and often have sole responsibility for their patients, yet they are paid less. Equitable pay is critical in attracting talent, and it is a primary focus of our legislative efforts in Minnesota.
 DME professionals have an opportunity in the pediatric home care market.
DME professionals have an opportunity in the pediatric home care market.Prove Value with Improved Evidence Base
Health care organizations and policy makers need data to make informed decisions on how to best deliver home care services to children with special health needs. While there is a national database of Medicare patients, that type of information is fragmented in the pediatric market because Medicaid systems differ state by state. In the adult world of home care, there are clear measures of health improvement—the ability to walk independently or feed oneself more reliably, for example.
Outcomes measurements differ in the pediatric world where kids are continually growing. We often begin with an infant incapable of supporting life without help and then progress through all kinds of normal development processes to reach appropriate milestones. An adult can be in a bed or wheelchair and use short ventilator tubing, while a child needs to roll, crawl and then walk to develop, so the equipment has to be configured differently to allow for that movement. In pediatrics, we need to get kids over different hurdles—getting them to eat, helping their brain, lungs, and heart develop, and allow for—in some cases—weaning off technology completely, whereas the aging population is likely to become more reliant on machines over time. Families often measure success by how long it's been since their children have been admitted to the hospital, and for some, that's been more than a decade.
There is significant evidence that pediatric home care is a cost-effective, patient-preferred alternative to hospital care with demonstrably positive outcomes. But there is a woeful lack of nationwide, comparable data that is needed to truly quantify the benefits of pediatric home health care overall. Research will require collaboration to compile sufficient data on hospital and home health care service utilization, re-hospitalization rates, costs and other factors.
Integrate a Fragmented Health Care System
As an industry, we must determine how pediatric home health care can align and integrate our services into new, more collaborative models of care. That includes identifying funding priorities that focus our resources on efforts that truly improve population health, reduce costs and improve patient experience.
The future of pediatric home care—and sustaining safe, effective, and affordable health care for all Americans—depends upon tearing down walls, eliminating redundancies, and working with others to optimize and share technology, information and precious resources.
Health care is going home, and not only because it is generally the patient-preferred environment. As the U.S. health care system changes to improve the health of its population, lower total cost of care, and improve the patient experience, home-centered care is a key solution in achieving that Triple Aim. As an industry, home care agencies must work together to design a new system that will safely meet patient needs today and in the future. That includes collaborating to define and differentiate these services, demonstrate their value with quantifiable evidence, and ensure fair payment to support sustainability. Meeting these challenges will determine our role in the future of health care, and enhance our ability to contribute to an improved, more integrated health care system.
