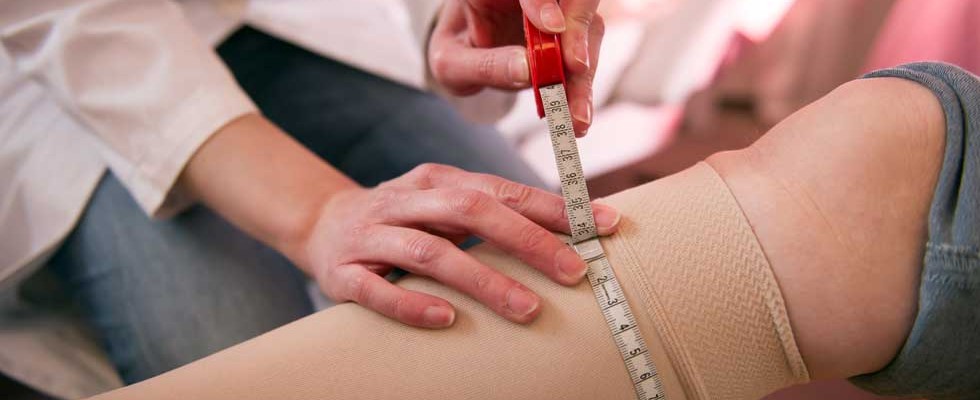
Compression therapy is key to the management of edema and is critical to boosting healing rates in venous leg ulcers (VLUs), acting to reduce venous hypertension and improve the flow of fluids in the lower extremities while standing and walking. Long-term use of compression is important to preventing ulcer reoccurrence.
Good circulation is vital to good health by providing tissues with nutrition needed to maintain strength and structure. Muscle contractions work together with the valves in lower leg veins to pump blood back up to the heart. Weakened valves in leg veins that do not close properly allow gravity to move blood in a downward flow that can pool and cause the vein to stretch or leak out into surrounding soft tissues, causing swelling or edema in ankles and legs.
Compliance challenges have been well-documented with use of standard compression devices. Patients become noncompliant when a device is difficult to put on or the garment is uncomfortable to wear for long periods of time. Without compliance, ulcerations do not heal properly and can lead to more serious complications. Comfort and the acceptability of the compression device is essential to its continued use.
Overcoming Application Difficulties
A wide variety of devices exist to provide compression for the long-term management of chronic edema. The most effective level of compression to overcome venous hypertension has been determined to be around 40 mmHg (millimeters of mercury) at the ankle. To achieve an appropriate compression level, the bandage should be applied at a consistent tension and be able to keep its shape over time. When patients, such as those who are elderly or obese, have physical difficulties applying their compression garment or are unclear on how to properly apply their garment independently, they can experience frustration, which often leads to noncompliance.
Proper application of compression therapy can determine the efficacy of compression. A cross-sectional study was conducted into whether homecare nurses were regularly able to achieve therapeutic levels of sub-bandage pressure using various systems, and the results showed substantial variation in exerted pressures, ranging from 11 to 80 mmHg (30 to 50 mmHg is considered optimal). When applying a two-component bandage, 63% of participants achieved pressures within the optimal range, while 41% achieved optimum pressure when applying an elastic bandage and 40% when applying an inelastic bandage. The study demonstrated difficulty achieving desired sub-bandage pressure when homecare nurses applied the bandage, indicating that a substantial proportion of patients do not receive adequate compression therapy. It also raises questions about the expectations put on patients to maintain proper compliance on their own.
Addressing Comfort
For compression to be effective, the garment must also be comfortable to wear and provide consistent, sustained therapeutic compression. Poor tolerance for wearing compression garments may contribute to reduced compliance, which reduces healing rates and may double the time needed to complete healing. The garment must be easy to use, with simple, quick application and removal; it must stay in place while worn.
A lack of air permeability in compression garments may cause the overheating of underlying tissues and excessive sweat production secondary to poor moisture exchange. A compression garment that is air permeable allows for the movement and transfer of air and heat to provide comfort that encourages longer wear and prevents the type of overheating that can result in sweating and skin breakdown.
A study conducted by an independent testing laboratory using the ASTM Standard D727, 2004 (reapproved in 2016), “Standard Test Method for Air Permeability of Textile Fabrics,” compared the air permeability of five leading compression garments used for the management of edema. The study illustrated the differences in the average amount of airflow for each option, suggesting the thermo-physiological effect of providing greater heat transfer and moisture or vapor transmission. A greater thermal equilibrium between the human body and the environment can improve comfort and overall compliance.
Studies show that the use of compression in compliant patients can increase healing rates for ulcers and reduce reoccurrence. It is essential to educate patients about the need for long-term use of compression and proper application to achieve appropriate compression levels.
Velcro & Bungee Garment System Compliance Study
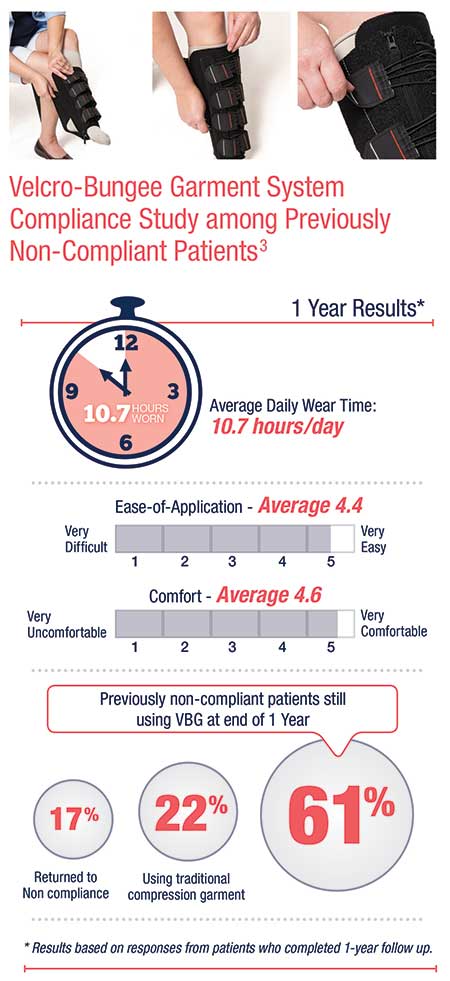
Lambert, et al., evaluated the ease of application, comfort and compliance of traditional compression garments compared with the use of a Velcro-bungee compression garment system.
Participants included patients who had previously demonstrated poor compliance with standard compression stockings or multilayer compression therapy. Those who had been noncompliant with traditional compression garments showed increases in both the length of use and in compliance, with 61% of the previously noncomplaint patients still using the Velcro-bungee garment at one year. On a scale of 1 (very difficult) to 5 (very easy), the average patient rated the ease of application at 4.4 at one year. Comfort received an average rating of 4.6 on a 5-point scale. The study concluded that the majority of previously noncompliant patients remained compliant at one year and used the system for an an average of 10.7 hours per day (see graphic).
Making a Difference
The benefits of compression for healing venous leg ulcers and reducing reoccurrence rates have been well documented in the medical literature, but this therapy can only work when patients comply with the protocol. By prescribing compression garments that address and reduce the two primary barriers to compliance—difficulty with application and discomfort—health care providers can significantly increase compliance rates, leading to reduced edema, improved wound care outcomes and a better quality of life for patients.
Regina Anderson is employed at AMERX Health Care and has been in health care management for over 30 years.
