An increasing number of Americans has difficulty keeping doctors’ appointments, which compromises their health and can lead to future medical crises.
In this country, approximately two million people are homebound, and many more lack the strength, resources or organization to regularly attend doctors’ appointments.
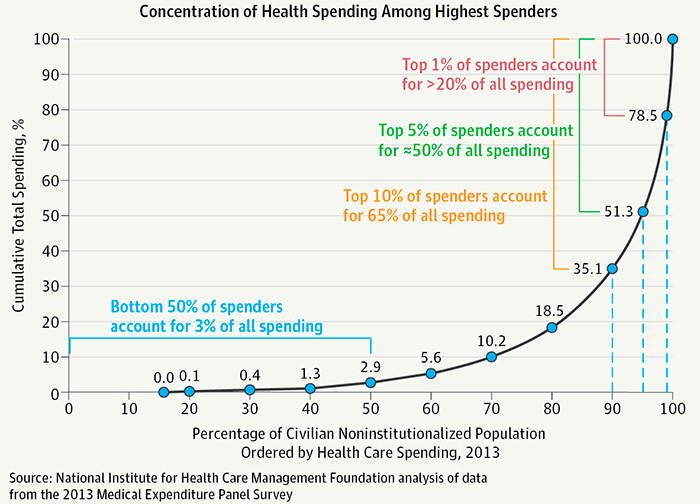
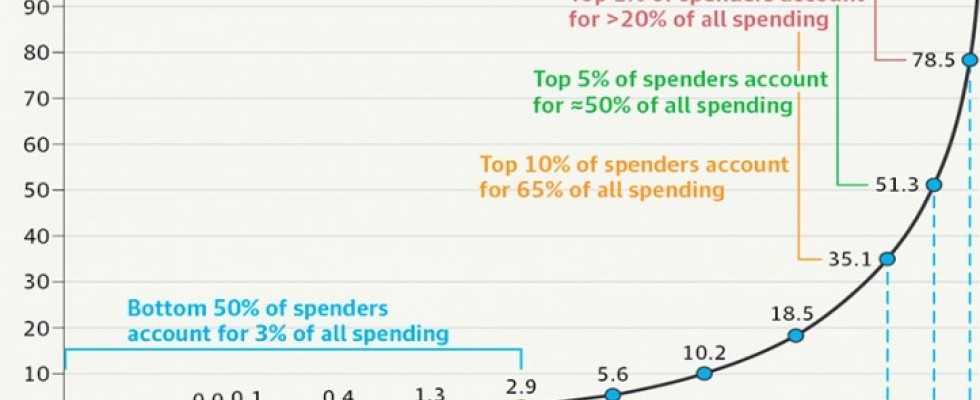
These are precisely the people who most need consistent care to manage their medical conditions. Without regularly scheduled, attentive care, they are likely to require multiple visits to the emergency room and more admissions to the hospital. Just 1 percent of people account for more than 20 percent of health care costs, and 5 percent drive half of all medical expenditures. Leaders of many of the country’s largest health care foundations recently made a combined plea for new models to care for these high-risk, high-use patients.
Home Sweet Home
Several home-based medical care programs have demonstrated improved health outcomes for homebound and high-risk individuals, and some have also been shown to reduce hospital utilization and cost.
Bringing care into the home reaps many benefits. These include the elimination of barriers that prevent traveling to appointments; enabling clinicians to understand how patients live; opportunities to assess why they may be failing physically; and identifying approaches and best practices for adapting care.
Unfortunately, the country faces a severe shortage of homecare providers. The 1.7 million home primary care visits conducted for Medicare fee-for-service beneficiaries in 2013 fall far short of the medical needs of the two million homebound individuals. There are many more whose care would be improved by treatment outside of traditional medical offices, though these patients are not, strictly speaking, homebound. Because few physicians choose primary care careers, and only a tiny share of those opt for home-based practices, the shortage is large. In fact, less than 500 clinicians performed 44 percent of those 1.7 million Medicare visits.
Telemedicine: The New Medical Frontier
Expanding homecare throughout the nation is an urgent priority. Telemedicine, quickly becoming a proven method for delivering health care across distances, could help alleviate the homecare shortage. In other clinical settings today, telemedicine programs allow specialists to perform consultations between hospitals, care to be delivered to remote populations and urgent care to be offered to employees at their workplaces. Telemedicine can be used for complex and homebound patients wherever they live.
A variety of new models of telemedicine are likely to proliferate in the coming years. Some models will primarily rely on home monitoring services linked to a nurse or other clinician to track physiological parameters. Many companies are developing or already offer this type of equipment; some also include remote clinical management in their offering.
Other programs might provide patients with secure video conferencing equipment and possibly diagnostic tools, and request that they link to their physicians for scheduled appointments. Equipment required to support true medical visits—as opposed to videoconferencing—is making its way into the marketplace. Some integrated delivery systems are experimenting with such virtual visits.
A third model sends a non-physician into the patient’s home and links to a remote primary care provider (PCP) using telemedicine equipment. The in-home provider can build trust, observe the home environment, manage care and operate telemedicine equipment for the remote PCP. This approach enables a richer medical visit than remote programs lacking personnel in the home.
Each of these homecare telemedicine strategies has distinct advantages and potential challenges. The ideal model in each setting will likely be determined by the needs of the population, resources available and program goals.
Another program decision of telemedicine-enabled homecare services is the selection of remote PCPs. Some programs may wish to use a patient’s current PCP, extending that existing relationship into the home. This has obvious advantages in terms of continuity of care, patient familiarity and access to an existing cadre of clinicians. Other programs may opt to assign a new physician—one who specializes in caring for this challenging population and understands how to make full use of the technology platform. Here too, the decision will likely be driven by available local resources and program needs.
Tools for Success
The new generation of technology makes house call visits more scalable and affordable. No matter how care is brought into the home, the following elements are key when developing a home-based telehealth program:
- Patient Selection: The first step to success is identifying those patients most likely to benefit from home-based care. Patients with high levels of need that are not receiving consistent, coordinated, patient-centered care through the traditional delivery system are ideal candidates. They may have many chronic illnesses or specific groups of diagnoses that predict future need. The best way to find the patients for home-based care is to combine traditional methods that mine utilization patterns and diagnoses with patient-centered evaluations of self-management skills and social support networks.
- Patient Outreach: Communication that builds trust with patients and their caregivers is important to success. This requires creative strategies to connect with hard-to-reach patients, patient-centered engagement strategies and self-management support that is built around the patient’s perspective.
- Clinical Practice Guidelines: As a program grows, an evidence-based practice model for all clinicians ensures consistent, high-level care. That starts with clinical practice guidelines and can be reinforced through clinician training, education and outcomes reporting.
- Coordination of Care: Sharing clinical information among specialists caring for the patient (within and outside of the telemedicine program) helps create continuity and quality in a home-based delivery model. By sharing clinical information across providers, through a health information exchange or other means, improves the care process.
- Equipment: More advanced and higher quality equipment has improved communications and diagnostics for home-based visits. There are many HIPAA-compliant videoconference platforms available to connect all participants engaged in a telemedicine session. The market for mobile diagnostic equipment continues to expand, opening possibilities for more in-home care.
- Logistics: For programs that deploy providers into the home, a significant source of inefficiency is drive time. Companies such as MedZed, among the first to offer in-home care through a network of mobile medical professionals linked by telemedicine to remote PCPs, rely on logistics to address the challenges of distance, traffic and provider availability.
The Future of Telemedicine
About 10,000 people in the U.S. turn 65 every day. According to the Centers for Medicare & Medicaid Services, there are 125 million Medicare and Medicaid beneficiaries in the U.S., and that number will increase dramatically in the coming years. As CMS moves more reimbursement to value-based payments and commercial insurers follow, provider organizations and health plans will need to find new cost-effective models to care for patients. Telemedicine is one solution.
The combination of our aging population, the rise in health care costs, and rapidly evolving technology suggests significant opportunity to expand home-based telemedicine care in the U.S. For this emerging set of solutions to succeed, we need openness to new models of care among physicians and patients, along with reimbursement systems that reward keeping people healthy. The next decade will likely be a time of great innovation, as new models of care are tested that hopefully provide benefit to the neediest patients.
