
Having access to home respiratory care is not a luxury for seriously ill patients; it’s often a lifesaving necessity. For the millions of Americans struggling with respiratory diseases such as chronic obstructive pulmonary disease (COPD) and obstructive sleep apnea, home respiratory care is vital for improving health outcomes, quality of life and independence—all in the comfort of their own homes.
At the same time, access to oxygen therapy in a home-based setting is creating efficiencies in the Medicare system and saving taxpayers billions of dollars—a rare win-win. It is increasingly preferred by patients, providers and policymakers alike. Yet despite the advantages it brings, many people don’t fully appreciate the importance of home respiratory care.
A Patient-Centered Approach
Home respiratory care is a convenient, effective and patient-centered way to provide high-quality services and supplies to help patients breathe easier. But perhaps more importantly, it is life-sustaining therapy that allows patients to remain in their homes. Once a physician prescribes respiratory therapy, many patients receive oxygen supplies and therapy services in their own homes, rather than in inpatient settings such as hospitals and nursing homes.
Home respiratory care providers offer patients therapy services, including comprehensive education about managing their disease and respiratory equipment, and quick delivery for medical devices. In addition, many patients receive regular follow-up services from respiratory therapists who come into the home to conduct evaluations, ensure equipment is fitted and functions properly, and continually educate the patient and caregivers about optimizing outcomes.
If required, patient service technicians will visit the home to provide detailed instructions about home oxygen supplies and equipment, evaluate the safety of equipment and the patient’s home environment, and empower the patient to confidently and correctly use the equipment. Such one-on-one services are critical for ensuring adherence to physician-prescribed respiratory treatments.
Who Needs Care?
Because they are extremely vulnerable, patients with serious respiratory illnesses such as COPD need home respiratory therapy to maintain their quality of life. As the third-leading cause of death in the United States, COPD affects an estimated 15 million Americans, and as many as 12 million more suffer from the disease but are not yet diagnosed. Among Medicare beneficiaries, research suggests that 12% have COPD—a number expected to grow as Medicare’s population expands.
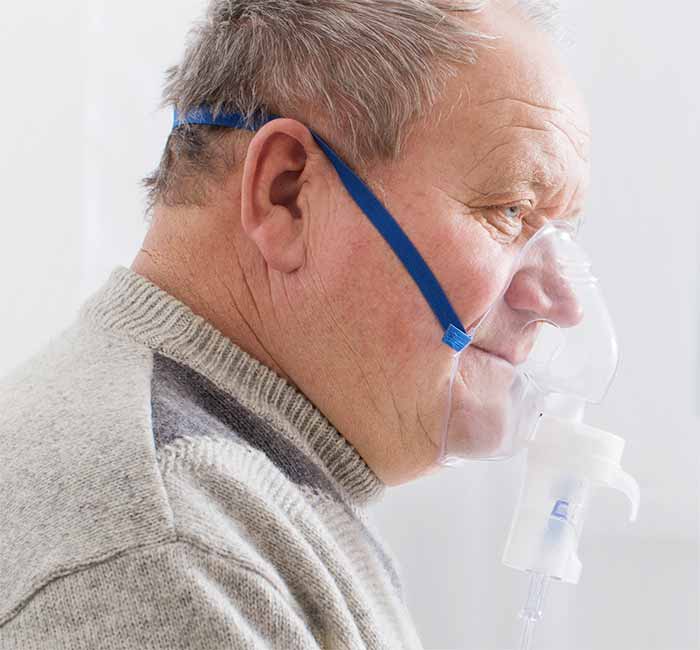
COPD is not a singular disease; it encompasses a variety of respiratory illnesses including emphysema, chronic bronchitis and refractory asthma, which is irreversible. Characterized by increasing breathlessness, COPD causes patients to feel extreme tightness in their chests, to cough and wheeze (sometimes violently), and to feel as if they cannot catch their breath. Though there is no cure, COPD can be managed effectively with home respiratory therapy.
As their lung functions deteriorate, many people are unable or unwilling to leave their homes lest environmental factors such as pollen or air pollution make it even harder to breathe. Some patients struggle to get around on their own, as even walking can lead to severely labored breathing. Not all patients are homebound, however, and even those who are can lead more independent, fulfilling and mobile lives with the proper care.
Seeing the Full Picture
Because it happens outside the confines of a physician’s office or hospital, it is easy to overlook home respiratory care or underestimate its importance. But that would be a mistake. Home respiratory care is critical to helping patients live longer, healthier lives, and also lowers costs for the nation’s health care system as a whole.
In fact, home health care is a medically- and cost-effective alternative to hospitalization for millions of Medicare patients. According to a recent study published in the American Journal of Accountable Care, patients who are treated in a home-based setting are significantly less likely to be readmitted to the hospital. Moreover, patients who receive home-based care services are less likely to visit the emergency room than those treated in the hospital.
Not only do patients treated at home tend to be healthier than their hospitalized peers, but the improved health outcomes also have a positive effect on health care spending. Research shows that the average costs for patients treated in a home-based setting is $13,000—35% less than patients treated in inpatient settings, which totals $20,325 on average. The estimated annual cost of COPD for 2010 was $49.9 billion; home respiratory care can make a significant dent in that spending while improving patient outcomes. As more patients choose to receive oxygen supplies and equipment at home, hospitalizations and emergency room visits are expected to drop even further, generating substantial savings for Medicare and taxpayers.
Perhaps most importantly, home respiratory care is preferred by patients. Like most Americans, COPD patients value the option to be treated in the comfort and privacy of their own homes. This is especially true for patients who live in rural and underserved areas or who have difficulty accessing transportation. One study suggests that more than 3.6 million Americans, many of whom are Medicare beneficiaries and oxygen patients, miss medical appointments due to lack of transportation—a trend that can be alleviated by home respiratory care.
Despite the clear benefits of home respiratory care, federal regulations threaten to undercut vulnerable patients’ access to certain home treatments such as non-invasive ventilation (NIV). Used by a small number of critically ill patients, NIV supports patient health, independence and the ability to remain at home near friends and loved ones. Yet policymakers recently included NIVs in Medicare’s competitive bidding program without first testing the impact of the new method for bidding in that product category. Competitive bidding has already led to lost access to specific services, including respiratory therapy, and the new NIV regulation puts patient access at risk since it is unclear how the market will react to supplying ventilators at an affordable price to patients in need.
There is real fear. Several peer-reviewed articles found that when liquid oxygen was subjected to the competitive bidding program, many patients across the country suddenly couldn’t access the therapy they needed to survive. Without the necessary caution and prudence to observe how the revamped competitive bidding program will operate in practice, it is unclear how many patients may lose access to lifesaving equipment such as NIVs at home.

Shaping the Future
The value of home respiratory care should not be underestimated. Health care influencers shaping future payment reforms for our sector need a clearer understanding of the role we play in the lives of the patients we serve. Collectively, the HME industry helps more than 1 million Medicare beneficiaries remain in the home while maintaining quality of life and managing their disease. Let’s all remember to underscore that value among those who matter most to our future: patients and payers.
Payment Reforms Underway
New Medicare payment policies could threaten patient access to oxygen therapy supplies and services. The Centers for Medicare & Medicaid Services (CMS) finalized a regulation late last year that implements reforms to the competitive bidding program for durable medical equipment, prosthetics, orthotics and supplies (DMEPOS)—including home oxygen supplies and equipment.
While CMS’s latest action takes positive steps to reform the competitive bidding program—steps commended by the home respiratory care sector—providers remain concerned that specific aspects of the program will continue to create access problems for patients.
Also, the competitive bidding program remains incredibly complex and there is great concern that not all providers understand the new process, which could lead to artificially high or low payment rates. If that occurs, providers could be forced to exit the market altogether, further restricting patient choice and access.
To ensure that the provider and supplier sector is prepared to understand and participate in the bidding process for 2021—set to open in July—tools have been developed to educate and inform providers about the new bidding program and how it will impact their business. Further, by utilizing these online tools, providers can ensure they are bidding fairly and accurately.
