Home health care professionals frequently encounter patients with COPD—no surprise, considering 16 million Americans are diagnosed with the chronic respiratory disease, which is the third-leading cause of death in the United States.
But some obstacles for COPD and other pulmonary patients can be mental, not physical, said Megan McMurray, a clinical psychologist who works with patients while they’re undergoing pulmonary rehabilitation. Mental health concerns are common in patients with chronic pulmonary disease, as the prevalence of anxiety and depression is higher in these patients than in the general population. While estimates vary widely, research suggests that 13%-50% of pulmonary patients have symptoms of anxiety, with some estimates as high as 74%. Estimates for depression symptoms in patients with COPD range from 15%-35%, and as high as 49% for patients with interstitial lung disease.
“A significant portion of patients with pulmonary disease struggle with anxiety or depression symptoms,” said McMurray, who is an assistant professor at the University of Alabama at Birmingham School of Medicine and president-elect of the Southern Association of Cardiovascular and Pulmonary Rehabilitation. “They may not always meet the diagnostic criteria for a mood or anxiety disorder, but they’re having the symptoms and that adds to the burden of the disease.”
A Difficult Diagnosis
Mental health struggles are tied to higher exacerbation rates and more frequent hospitalizations. As part of a team of caregivers at an outpatient cardiopulmonary rehabilitation center—where about half of the patients have significant respiratory problems—McMurray and an interdisciplinary group work to remove those obstacles.
Just getting the news about having COPD or another chronic pulmonary condition can be a huge mental load for patients, she said. In the initial days and weeks after diagnosis, they may struggle to come to terms with their new reality.
“It’s a lot to take in, knowing this is going to be chronic, it’s going to be a challenge, and a lot of the time people didn’t even know they were sick,” she said.
Additionally, many newly-diagnosed patients have experienced some level of restriction in their daily activities—giving up their outdoor hobbies, exercise and even their jobs—and are suddenly more isolated within their homes.
“One of the most common mental health complaints in these patients is: ‘I used to do these fun things and I cannot do them anymore because I do not have the energy and/or I get too short of breath,’” McMurray said. “It’s very important for people to get outside their homes and engage in some type of activity.”
Making it worse, the physical symptoms of the disease, such as shortness of breath and fatigue, can also trigger mental health symptoms like anxiety or panic. After all, feeling as if you can’t breathe causes worry for everyone.
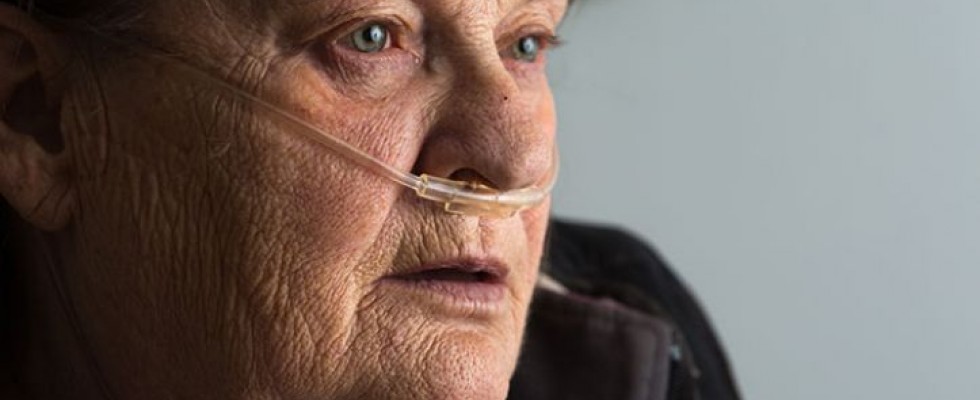
And even though those in the homecare business know that supplemental oxygen can significantly improve quality of life for those with COPD, patients are often resistant to or further depressed by the need for oxygen, which can represent a mental barrier for compliance and adherence in these patients, McMurray said.
“Patients often tell me that they are embarrassed or ashamed to wear their oxygen because they feel like it makes them look old or weak,” she said. “We have to work with patients to challenge these dysfunctional thought processes and replace them with more helpful thoughts.”
Ways to Help
Here are some things caregivers—including those without mental health training—can do to help:
1. Be a listener.
Individuals with pulmonary disease who lack adequate social support often have worse health outcomes. Caregivers can enhance the patient’s social support just by being a caring professional. This can be especially helpful when the patient does not have an adequate support network in place. Try to listen to patients actively and validate their feelings.
“You’re not taking the place of a friend or family member, but you’re there to listen, and that may mean a lot more than you realize,” McMurray said.
Often, she said, people don’t want to burden others with their feelings, so encouraging patients to use their existing social support networks (such as family, friends and communities) is also important.
2. Encourage activities.
One of the most crucial things caregivers can do is to encourage patients to find some way to continue doing activities they enjoy or to find new hobbies or interests to enjoy. That may mean finding modifications to make an activity safe and comfortable. For example, if someone loves to cook but finds standing in the kitchen too difficult, help them sit at the table to chop vegetables or pull a stool up to the stove to stir.
The most important thing is that they do something to keep engaged. It’s important for patients undergoing pulmonary rehab like McMurray works with, but it’s important in staving off depression for everyone. “We call this behavioral activation, but it’s really just doing things,” McMurray said.
3. Involve other caregivers.
If a patient’s mental health symptoms linger or worsen, consider referring them to a behavioral health specialist (such as a psychologist, psychiatrist or licensed mental health counselor) or checking with their attending physician to ensure their psychosocial needs are being met. In McMurray’s program, doctors, nurses, exercise physiologists, nutritionists and mental health professionals work together to treat the whole patient.
4. Work with the family.
Many patients lack social support, so educating families about how to help is critical, McMurray said. At her clinic, families are invited to participate in support groups, and they learn more about their loved one’s struggles as well as how to manage their own boundaries, spot depression and prevent caregiver burnout.
On the other hand, overly-concerned families can also present a barrier, she said, such as when a spouse, parent or child insists a COPD patient should remain inactive, McMurray said.
“They think they’re doing the right thing by saying, ‘Just sit down,’ or, ‘Go lay down, you’re sick, that doesn’t sound safe.’ They’re coming from a good place, but they’re encouraging the patient to avoid activity,” she said.
McMurray said that, despite the difficulties they face, working with patients going through cardiopulmonary rehab is one of the most rewarding things she does.
“I think it’s because there’s so much potential for improvement in these patients, who often come in very debilitated and feeling helpless,” McMurray said. “Watching them improve physically and mentally is so rewarding.”
