
Understanding reimbursement before change comes
Wednesday, September 4, 2019
Home health providers have become accustomed to dealing with the regulatory changes that come their way. In recent years there have been updates to the Medicare Conditions of Participation, new OASIS assessments and pilot programs testing out value-based care and pre-claim review models. And on Jan. 1, 2020, the Patient-Driven Groupings Model (PDGM) will overhaul the payment model for agency reimbursements—shifting thresholds for full payment, increasing billing frequency and tightening the connection between payment and the patient’s diagnosis, among other changes.
The new reimbursement model also dramatically increases the number of financial groupings that may result from a claim. The Centers for Medicare & Medicaid Services (CMS) has expanded the number of payment groups from 153 to 432.
The flow chart CMS created to describe PDGM shows why so many combinations of factors will impact payment. Five different variables each have multiple options that affect how the payment grouping is created. It is important to understand how these factors work together so you can determine the most appropriate home health resource group. This will make it easier to understand which factors make the most difference, helping providers anticipate reimbursements and align resources.
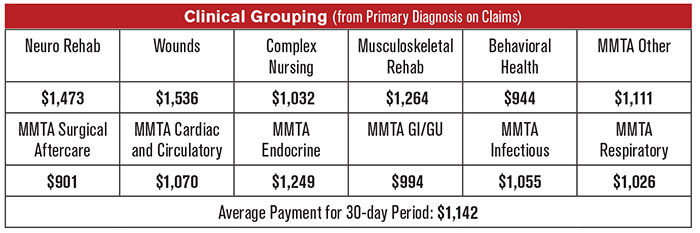 Figure 1: Clinical grouping based on primary diagnosis
Figure 1: Clinical grouping based on primary diagnosis
 Figure 2: Admission source and timing affect on payment
Figure 2: Admission source and timing affect on payment
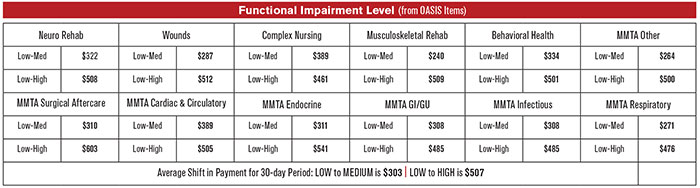 Figure 3: Adjustments for patient functional mobility
Figure 3: Adjustments for patient functional mobility
 Figure 4: Comorbidity adjustment
Figure 4: Comorbidity adjustment
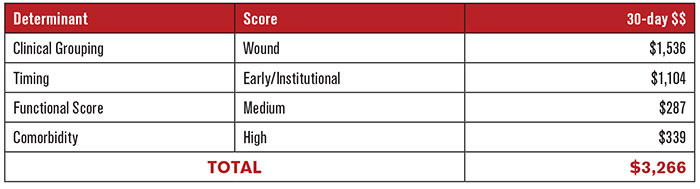 Figure 5: Example of reimbursement
Figure 5: Example of reimbursement
Baseline Payment Under PDGM
It is best to understand the baseline payment for each clinical grouping. CMS has configured PDGM so that reimbursements are based on resources needed to care for the patient. The minimum for each clinical group will be when a referral comes from the community, the timing of the episode is late, the patient is determined to have a low functional impairment level and there is no comorbidity adjustment. Figure 1 shows dollar amounts based on the $1,883 payment for a 30-day period that CMS has established for PDGM. The numbers reflect a labor rate of 1.0 and do not include the impact of the proposed 8.01% behavioral adjustment to payments. (The 8.01% payment adjustment is updated from an initially proposed adjustment of 6.2%.) There are 12 clinical groupings and a payment period is assigned to a grouping based solely on the primary diagnosis code submitted on a payment claim. Figure 1: Clinical grouping based on primary diagnosis
Figure 1: Clinical grouping based on primary diagnosisFactoring in Admission Source & Referral Timing
Beyond the minimum payment for a clinical grouping, the next factor affecting reiumbursement is the admission source and timing of the referral. CMS set up PDGM with financial incentives for providers to begin treating patients with more acute care needs first. This is the reason referrals from institutional settings are paid at a higher rate than those from community settings. The timing of each referral is also important because early and late referrals are paid at different rates. PDGM defines early episodes as the first 30 days of an admission, assuming that the patient was not treated under the home health benefit in the 60 days before the current admission. All subsequent 30-day billing periods will be considered late episodes and paid at a lower reimbursement amount. Figure 2 shows the amount that would be added to the baseline amount for the clinical grouping depending on the admission source and timing for the payment period. Figure 2: Admission source and timing affect on payment
Figure 2: Admission source and timing affect on paymentAdjustments for Patient Functional Mobility
The most recent revisions to Medicare’s OASIS assessment included additional functional assessment items. This was a precursor to the importance PDGM places on the functional mobility of the patient. Functional scores can change payments based on whether they fall into a low, medium or high impairment level. Within a clinical grouping, the reimbursement change is the same for an impairment shift from low to medium. However, the amount of the adjustment varies slightly between the different clinical groupings. The same is true for impairments that shift from low to high. The average shift for a 30-day payment period from low to medium is $303, while the average for a shift from low to high is $507. Figure 3 details the payment shifts for different OASIS items. Figure 3: Adjustments for patient functional mobility
Figure 3: Adjustments for patient functional mobilityComorbidity Adjustments
The last payment factor introduced with PDGM is the comorbidity score. A claim can contain up to 24 secondary diagnoses. There are approximately 1,100 codes, which, if included on a claim as a secondary diagnosis, would qualify the payment period for a low comorbidity score. CMS has also created listings for pairs of codes which, if included as secondary codes, would lead to a high comorbidity score. This is expected to happen about 10% of the time. Several diagnoses result in these high comorbidity adjustments. For example, a patient with diabetes and Parkinson’s disease would have a high comorbidity; a patient who is bipolar and has ankle ulcers would as well. Home health operations experts who have studied PDGM closely will have lists of combinations resulting in a high comorbidity adjustment. It is imperative that providers adhere to the Conditions of Participation when identifying a patient’s diagnoses. The codes listed should relate directly to the work that will be done during the course of care. Additionally, all work must be properly documented. Figure 4: Comorbidity adjustment
Figure 4: Comorbidity adjustmentExample of a Grouping Calculation & the Reimbursement
When these numbers are combined, the result shows how each factor works together to impact the reimbursement. For example, a wound patient referred from an institution who has a medium functional score and high comorbidity would result in a $3,266 payment for the first 30-day period. Figure 5 shows an example. If the patient’s condition did not change dramatically during the first 30 days, the second 30 days would be deemed a late/community episode and payment would be reduced by $1,104 to $2,162. Figure 5: Example of reimbursement
Figure 5: Example of reimbursement