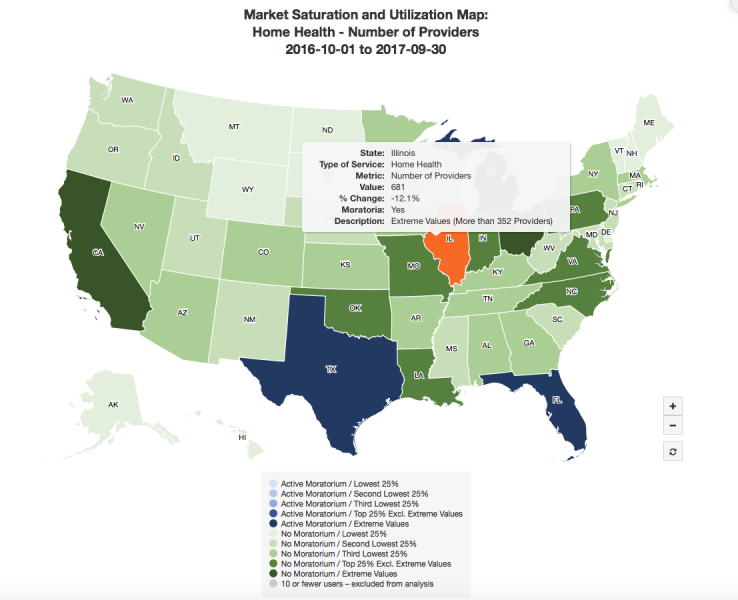
(November 1, 2018)—The Centers for Medicare & Medicaid Services’ Market Saturation and Utilization Data Tool is one of many tools used to monitor and manage market saturation as a means to help prevent potential fraud, waste and abuse. It also assists health care providers in making informed decisions about their service locations and the beneficiary population they serve.
Data analysis pulled through the Market Saturation and Utilization Tool is based on paid Medicare Fee-for-Service (FFS) claims data from the CMS Integrated Data Repository (IDR). Metrics include number of fee-for-service beneficiaries, number of providers by type that includes home health and hospice among others, average number of users per provider, number of dual eligibles, total payment and more.
Claims are used to define the geographic area(s) served by a provider rather than the provider’s practice address. Further, a provider is defined as “serving a county” if, during the 12-month reference period, the provider had paid claims for more than 10 beneficiaries located in a county. A provider is defined as “serving a state” if that provider serves any county in the state.
While this tool does not include information on market saturation and utilization for Medicaid or private insurance, it does include an interactive map that is color-coded based on analysis. For those interested in states and counties affected by CMS's temporary provider enrollment moratoria during the reference periods for which data are available, the interactive map identifies those states and counties.
This 8th Release is an update from Release 7 and also includes preventive health services data and two additional reference periods.
Use the Market Saturation and Utilization Data Tool here.