Dealing with pain takes more than endurance; for chronic pain, it requires strategy and persistence. Pain relief is a long-term project, but with an understanding of the nature of pain and new tools, managing pain can actually be easier at home than in a health care setting.
Unfair Warning
Pain is a complex array of causes and consequences. It acts as an alarm system, notifying the brain of danger, much like a motion detector around a vulnerable window. With persistent threats, more and more alarms are installed in an attempt to keep the location safe. But alarms may become so sensitive that they still go off even after the cause of the danger is gone. While physical alarms can be uninstalled, dismantling the warning signals created by chronic pain is less straightforward.
Chronic pain physically changes the brain. For example, before knee replacement, the thalamus enlarges from processing large amounts of pain. Within six months of a bad knee—and the pain—being removed, the thalamus returns to normal size. For pain without that kind of quick fix, treatment must include retraining the brain to cope with sensations that aren’t actually threats.
Distraction Helps
Pain scales are great for rating pain in acute or emergency situations where a treatment and change are eminent. In that case, knowing that a dose of medicine lowers a patient’s pain from an “8” to a “3” is useful. At home, however, constantly rating pain draws focus to it, magnifying the brain’s perception. Pain eases when focus is placed on something else.
In order to manage pain at home, it’s also important to make a plan. Pain without a way to treat it leads to fear and vulnerability. Fear increases the perception of pain and makes it hard to focus on anything else.
In a more intense form, fear of pain is sometimes called “catastrophizing.” All the possible ramifications of untreated pain run through the mind, leading to depression, fear of attempting activities and lack of movement. Studies show that people who tend to catastrophize require more pain medications, are more likely to become addicted to medication and take longer to heal.

Addressing Pain
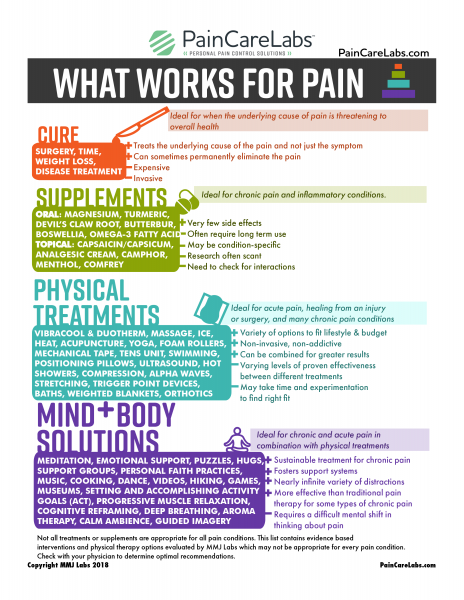
With home management, there is not a single solution. In fact, research shows that almost every treatment—from pills to physical to psychological solutions—decreases pain by about 30%. The trick for pain management is making a pain plan that layers solutions, and provides multiple options for breakthrough pain or bad days. Add 30% reduction to 30% reduction to 30% reduction, and pain is significantly reduced.
Here are some of the options:
Medication:
Multiple studies on oral surgery and fracture recovery have shown that ibuprofen is superior to most kinds of opioids for pain. A doctor should advise on medication management and pain relief.
Over-the-counter supplements:
Magnesium, for example, is frequently low in patients with chronic pain. It’s a great anti-inflammatory and smooth muscle relaxant and even blocks the N-methyl-D-aspartate receptor, assisting with pain relief. For patients on opioids, magnesium can help get the same effect with a lower dose.
Sleep management:
When pain or worry impacts sleep, pain becomes more of a burden the next day. Whether supplements, over-the-counter medicines, prescriptions, or meditation, warm baths, exercise, or a better pillow or mattress work for your patient, sleep is key.
Neuromodulation:
Pain and other sensations are transmitted to the spine, modified, then interpreted and inhibited in the brain. Impacting nerves directly before pain gets to the brain is called neuromodulation. While there are implantable electrical neuromodulation stimulators that directly impact transmission, you are practicing neuromodulation every time you rub a bumped elbow or run a burned finger under cold water.
Gate control devices:
This stems from the idea that sending a lot of motion messages through the spine slams a gate shut so the weaker pain signals can’t get through. Options include stimulating light touch, pressure and tension. Transcutaneous electrical stimulation, or TENS, units trigger sensations by transmitting electrical current flow. At low intensity, it triggers light touch receptors for continuous low-level pain relief.
More intensive stimulation:
Stimulating the Pacinian corpuscle pressure receptor—through roller balls, myofascial trigger point therapy, foam rollers, vibration and TENS units at high—inhibits pain more strongly. TENS units have to be turned up high enough to twitch the muscle, which may be uncomfortable for some. Vibration, because it is motion, can stimulate this receptor more comfortably.
Tapes and stretching:
Kinesiology tapes stimulate Ruffini corpuscles with stretching. Physical stretching, such as with yoga or Pilates, reduces pain the same way and increases blood flow. Tapes can also reduce pain over time by taking pressure off some areas and re-orienting the way muscles move. This removes irritation from injured areas by moving the strain to a different location.
Massage and vibrations:
Massage stimulates both pressure and stretching receptors and can reduce re-injury by separating muscle fibers more efficiently than stretching alone. Vibration from a massage wand or other device can also reduce delayed-onset muscle soreness by separating stiff muscles so that they are not injured with movement.
Descending noxious inhibitory control:
Ice or other slightly uncomfortable signals like prolonged pressure are assessed in the brain. When they’re not a threat, the brain will send pain-inhibiting signals that impact the whole body. For musculoskeletal injuries or overuse syndromes like tennis elbow, ice can reduce the production of the pain and inflammation triggers.
Mind-body pain relief:
For certain pain conditions like Raynaud’s disease, postherpetic neuralgia or chronic regional pain syndrome, the issue is not the muscles but in the nerve itself. For these conditions, stimulating muscles around the nerves may cause even more pain. For diffuse conditions like fibromyalgia, specific targeting may not be effective. In these situations, mind-body pain relief may be the most critical part of a pain plan. Studies have found that accepting pain and committing to focusing on valued activities actually reduces pain.
This “acceptance and commitment therapy” has elements that can work for everyone at home no matter the type of pain. Since movement and stretching help with all kinds of pain, committing to exercise at home is a distraction with several layers of benefit. Instead of focusing on the pain level, using goals such as leaving the house, chatting with friends or even watching favored shows can help by disabling the chronic pain focus in the brain.
Try Many Options
There is no one effective treatment for pain. For effective home management, investigate supplements, optimize over-the-counter pain relief, and make a pain plan for times when pain gets to be too much. Using devices that leverage as many receptors as possible can reduce pain in the short and long term. Focus on increasing the number of activities that bring joy, and don’t let the patient get discouraged.
