
“What!” you may be wondering after reading the headline. “2023?”
That’s right. Think of this article as tough love to help you make the right strategic and tactical changes today to meet the higher expectations and inevitable hindsight focus of future home health reviews by Medicare and others.
Doing nothing—or making only incremental changes—instead of using an innovative “greenfield” review is not an acceptable option when you consider these points:
- It will be three years before any changes started this year become productive.
- Higher 2023 requirements and expectations are already being put in place and are more likely to toughen than to weaken.
- If the last five years’ movement toward financial sustainability, transparency and second guessing have seemed relentless, you ain’t seen nothing yet.
A greenfield review takes a clean sheet of paper—think of a green, empty field—and reviews people, processes and facilities to improve immediate and long-term financial and operating results. Those without the right skills or attitudes, or whose salaries are above current market, are demoted, reassigned or receive employment-record impacts. It’s not a pleasant process unless you tackle the greenfield review yourself while your organization has time to change course. The goal is to better focus your limited financial and staff resources and create effective processes for change.
More Strategic Care Management
People with better access to transparent information will be judging your business come audit time. You need to know more than they do.
Imagine your organization’s 2023 external audit, assessment or peer review will be led by a big data analytics expert, a politician who sees health care as a winning topic and a health care plaintiff’s attorney. From there, make the following assumptions:
- They will have access to dramatically increased levels of information on costs, quality scores and best practices regarding processes and results for organizations of your size and for the very largest organizations.
- They will expect your home health organization to follow best practices and to have a relentless cost focus. They will concentrate on improved financial sustainability and patient engagement for highly visible critical-care conditions like COPD, diabetes, post-acute care and wound care.
- They will view 2019 best practices as entry-level expectations in 2023.
Knowing this is good for you, you want to estimate your future scores today and then work backward to see how you’ll rank when the test matters. Some want to ace this exam; others will be happy to survive.
Either way, use the following questions to gain more insight into how you can improve the quality of your care—with reasonable or even lower-cost options—in this era of heightened liability and pressures from all sides of the political and financial divide.
Your Home Health Framework
Create a framework for assessing your organization’s current status by starting with this simple two-minute exercise.
1. Answer the following two questions on a scale of 1 to 10.
First, look at your awareness. If a 10 means you could lead a 2023 home health panel discussion while feeling confident about the status of your patients and your staff performance, and a one means you aren’t comfortable with your preparedness, the condition of your patients or the performance of your staff, how aware is your organization of how to improve its home health care within reasonable investment levels?
Then, consider investment. If a 10 means you have conducted in-depth, sophisticated status and security overviews for patients and staff and you are already implementing all the recommendations to move toward the world of 2023, and a one means minimal investment to date and little budget available until next year or later, at what level is your organization investing?
2. Mark your answers on the two axes in the Home Health Awareness Versus Investment chart.
Mark your numerical answer for awareness on the horizontal continuum from “leader” to “novice” and your answer for investment on the vertical continuum from “reasonable investment” to “minimal investment.”
Draw a line between these two points to spotlight your home health awareness and suggest where to begin a strategic review.
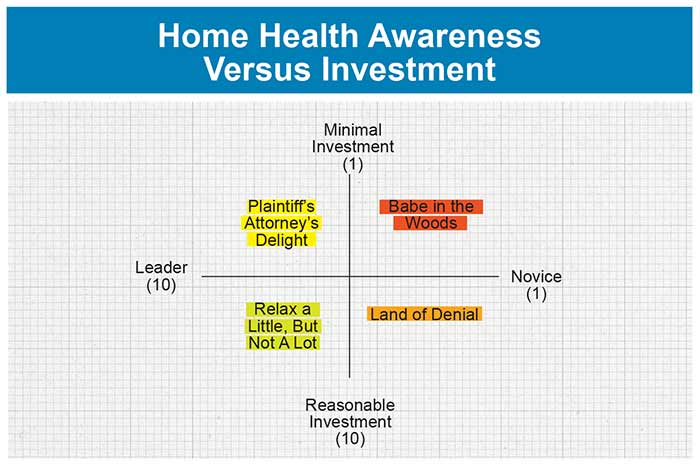
3. Consider the implications of your organization’s quadrant.
Babe in the Woods: The upper right quadrant suggests a limited or minimal budget for home health management and control, combined with limited or novice understanding of your security needs at the top management and board level. For you, data must be king.
Plaintiff’s Attorney’s Delight: Organizations in the upper left quadrant are aware of their opportunities and exposures, but still kick most cans down the road, addressing issues at glacial speed and hoping they won’t be attacked. Unfortunately, gold watches for lifelong tenure vanished long ago.
Land of Denial: The bottom right quadrant suggests a reasonable management budget, but only limited proactive appreciation of specific vulnerabilities that may originate from your supply chain and third-party vendors. Where can you reduce the number of ostriches hiding their heads in the sand when it comes to improving quality of care?
Relax a Little, But Not a Lot: The lower left quadrant suggests a strong understanding of strategy and operational home health issues beyond IT, along with executive-level commitment to manage risks and the accompanying political clout and resources needed. Reward the creativity of those who really move the needle—and not just with financial incentives.
If you are one of the fortunate few who are well ahead in terms of knowledge and addressing risks and opportunities, use this approach to determine your present situation and unearth your next opportunity. If you’re not so lucky, this is the time to estimate your 2023 ranking and identify the most crucial shortfalls.
A Call to Action
Health care organizations must provide value-based care, not just volume of care.
You probably recognize that what was considered good enough last year, as compared to the competition for your sector, size, company, etc., is not good enough this year, and will not be good enough in the future.
It’s a tumultuous world out there, but you can take steps to protect yourself from those wanting to claw back ever-dwindling reimbursements. Reduce your exposure to recidivism and readmission penalties and strengthen your ability to improve the quality of care for covered patients—which is why you went into health care.
You have until 2023 to make the changes needed for a good-to-great score. Your organization really can have the right answers for that review if you take advantage of your limited time rather than procrastinating. Your patients will thank you for the higher level of care they receive, and the reputation, job or organization you save may be your own.
