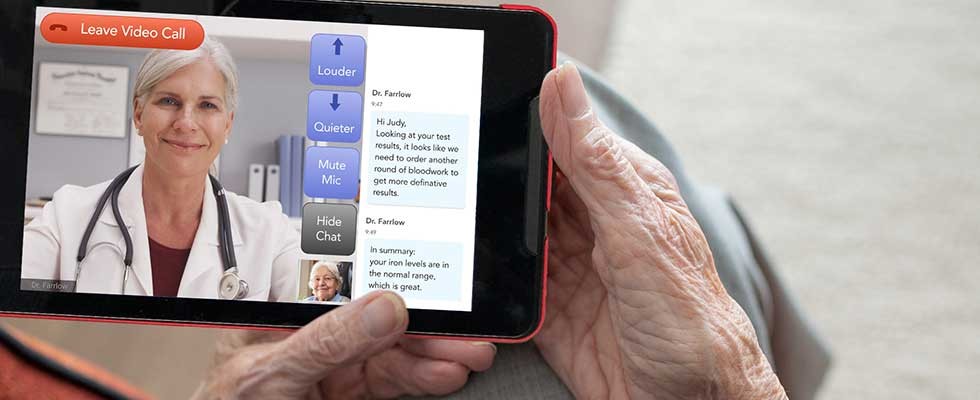
As home health care companies, nursing homes, hospitals, and clinics shut down to all but critical care needs when COVID-19 hit, two crises took hold across the country: reduced access to health care services, and increased loneliness.
Both loneliness and COVID-19 have the biggest impact on older adults. Whether living independently at-home, in an assisted living facility, or in a skilled nursing facility, access to care and needed social connection came to a swift and abrupt halt. Family members are prevented from visiting older adults and in-person doctor visits are being put on hold to minimize risk of contracting the virus.
This interruption of health care is especially problematic for people 65 and older, 85% of whom live with at least one chronic condition and who account for 80% of hospitalizations.
Interruption of social connections is also particularly problematic for older adults because loneliness in this age group can be a predictor of functional decline and death. Research shows that older people who are lonely have a 59% increased risk of losing their independence (as measured by activities of daily living, mobility, climbing stairs and performing upper extremity tasks) and a 45% increased risk of death.
Given these associated health care risks, it is not surprising that a study by AARP found that social isolation results in increased Medicare spending by an estimated $6.7 billion a year, thought to be due to increased inpatient care costs and skilled nursing home spending.
The Critical Role of Geriatric Medicine
Geriatric medicine is the field of medicine that specializes in health promotion, prevention, diagnosis, and treatment of disease and disability in older adults. The field encompasses medical conditions, as well as treatment for patients who suffer from falls, delirium, dementia, incontinence and support for medication management.
Geriatricians are trained to diagnose conditions that often present differently in older adults. They also develop care plans that address special health care needs, communicate with families and other caregivers, and coordinate care across settings in an effort to help seniors maintain as much independence as possible and a high quality of life—all of which is essential to effectively manage the physical and mental well-being of older adults.
This patient-centered approach focuses on the goals of each individual person. Geriatricians take the time to listen and hear their patients in order to balance the complexity of multiple conditions and quality-of-life preferences of the patients. This proactive, preventive and interdisciplinary practice area addresses many of the risks and common pitfalls of standard care.
Geriatrician, Laura Modqueda, MD summarizes the role of geriatric medicine, “My job is to help my patients be their best. It is important for me to understand the impact of health and illness on a patient and on those who love them. My person-centered approach to care necessitates understanding not only the medical problems a person may have, but also their emotional and social circumstance so that we are able to share in a decision-making process.”
COVID-19 Created a Chasm of Care
But what about patients who lack access to geriatric medicine? Consider, for example, a 90-year-old woman living in the COVID-19 environment. She has three chronic conditions: hypertension, atrial fibrillation and severe arthritis. Since her husband’s passing eight years ago, she has lived alone in her own home. Consider the patient’s caring physician who specializes in geriatric medicine. She would go to the ends of the earth for her patient. Our older patient needs guidance on the management of her conditions, but has been instructed to stay home. Her physician, committed to staying on top of her patient’s medical conditions, turns to digital solutions. The doctor has access to digital platforms for making video calls. However, the patient has poor internet connection, an outdated computer and a phone that is very hard to see because of her visual impairment.
The result is a chasm of care that impacts quality of care and outcomes for both health care, the physician, and the older patient.
Telegeriatrics Closes the Chasm of Care
Telegeriatrics is an emerging approach that blends technology with traditional geriatrics in ways that cater to the needs of elderly patients, while meeting the clinical needs of gerontologists or long-term care providers.
This approach has been gaining interest and adoption among caregivers because of the need to prevent unnecessary exposure to COVID-19 for elderly patients. In March, the Centers for Medicare & Medicaid Services further paved the way for the expansion of telehealth services for seniors by announcing that it would remove additional restrictions on telehealth reimbursement through Medicare, which covers 62 million Americans aged 65 and older.
Health care organizations that want to implement a telegeriatrics approach should understand the following:
- Telehealth for seniors is a reimbursable service. Previously, telehealth visits through Medicare had been restricted to older adults living in rural areas, for patients who had an already-established relationship with a provider, and for telehealth services that took place in a rural health care facility. This expansion will allow all Medicare beneficiaries to receive care in their homes through devices that enable audio and visual communication. It will also allow providers to bill for those services at the same rate as an in-patient visit, making it more likely that providers will adopt telehealth.
- Telehealth for seniors can impact health care spend. Telegeriatrics can play a critical role in managing health care costs, especially considering that 90% of the nation’s $3.5 trillion in annual health care expenditures are people with chronic health conditions and that 80% of the growing senior population have at least one chronic condition and 77% have at least two.
- Telehealth can help stop the spread of COVID-19 among caregivers and seniors. The implementation of telehealth is necessary not just to effectively serve the rapidly expanding patient population with COVID-19 but also to keep otherwise healthy seniors out of the hospital, while also protecting healthcare workers and caregivers.
- Telehealth is essential for preventing loneliness in seniors. The unexpected consequence of social distancing—loneliness—has severe, negative impacts on the health and well-being of older patients. When telegeriatrics employs technology platforms that enable clinical interactions and foster social connections for seniors, engagement increases, outcomes improve, and seniors remain happy and connected to the ones they love.
While age has often been cited as a barrier to the expanded use of telehealth, it’s becoming increasingly clear that older patients are willing to adopt technology that is safe, reliable and easy to use. When this technology is integrated into a geriatric medicine model it supports the growth of telegeriatrics, which benefits patients, families and health care organizations alike.
Dr. Kerry Burnight is Chief Gerontologist for GrandPad. A former professor of geriatric medicine and gerontology at the University of California-Irvine, Dr. Kerry founded the nation’s first elder abuse forensic center, as well as the national nonprofit, Ageless Alliance: United Against Elder Abuse. She can be reached at kerry@grandpad.net.
